By: Ana Maria Dumitru
Editor’s Note: This reflection and brief summary of a research[i] article was written by a future physician as part of an elective on fertility awareness with Dr. Marguerite Duane at Georgetown University College of Medicine. It highlights practical applications of charting the female cycle, a powerful tool underused by physicians and patients alike.
A Future Physician Learns About FABMs
I recently completed the FACTS elective for medical students. As with all my experiences with FACTS, I was surprised by how much I learned during this course. I learned more about the major fertility awareness based methods (FABMs) and the evidence base that supports them. I also had the opportunity to see how the basic knowledge FABMs provide can make such a huge difference in patients’ lives.
The Power of Charting the Female Cycle
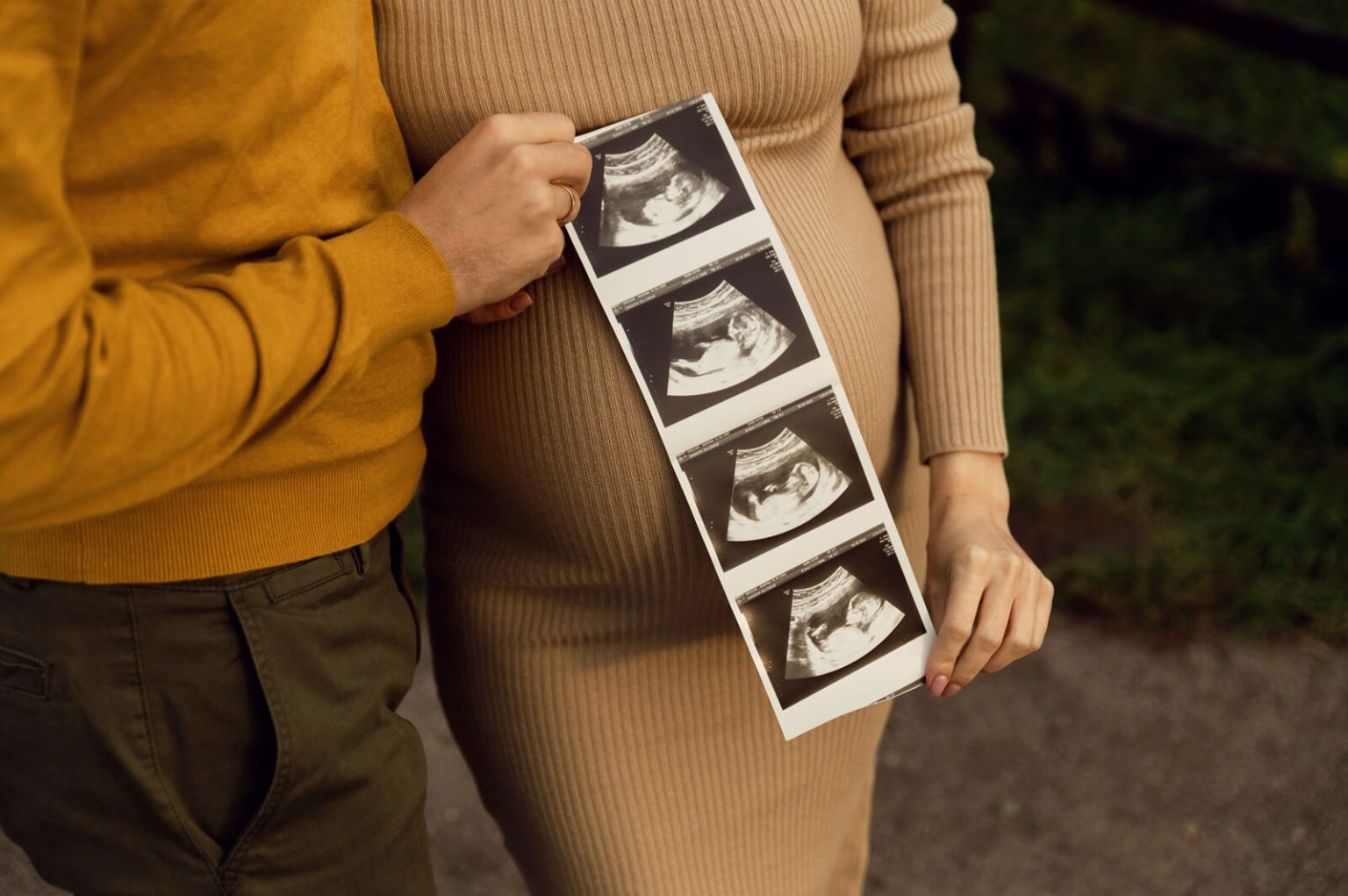
During one of my clinical experiences, I observed as Dr. Duane used a patient’s charting data to solve a clinical mystery that had befuddled two reproductive endocrinologists, four medical centers, and a complex care team over a span of three years. This patient had undergone an extensive infertility workup that probably cost her (and the healthcare system) tens of thousands of dollars (including an MRI, a hysterosalpingogram, and dozens of labs, office visits, and prescriptions). All the data from her workup was not sufficient to identify the underlying issue. It was also not enough to give her the pregnancy she so desired or at least provide the answer as to why she has been unable to conceive. Yet, when this patient was taught to chart her cycles (in her case, using the Creighton Model) and brought her charts to Dr. Duane, that all changed. Dr. Duane was able to solve the puzzle within an hour by piecing together her complex medical history in the context of six months of good charting data along with the results from the rest of this patient’s medical workup.
What If…?
This experience made me wonder, Wouldn’t it be great if every woman knew how to chart? Wouldn’t it be nice if every doctor who works with women of reproductive age knew how to interpret fertility charts? If that’s too lofty a goal, maybe doctors could at least know enough about charting to recognize it as a valuable point-of-care tool. For women who are subfertile or infertile, it seems like this could save them some serious heartache, time, and healthcare resources.
Research Supports Fertility Awareness
As it turns out, we have primary literature evidence to support this goal. Frank-Herrmann and colleagues published results from a prospective cohort study in 2017 in Archives of Gynecology and Obstetrics in which they followed women who had been trying to get pregnant for an average of 3.5 years (ranging from 1-8 years across all subjects). There was only one intervention: the study authors taught a group of women about their fertility and followed these empowered women for an additional eight months. They compared this cohort to a group of women with the same profile and infertility who were not trained about their fertility during those eight months. The researchers found that the women who were taught about their fertility had an almost double pregnancy rate compared to control subjects (38% compared to 21.6%). This result is without any other interventions! As the authors of the study conclude, “Training women to identify their fertile window in the menstrual cycle seems to be a reasonable first-line therapy in the management of subfertility.” So if you know anyone struggling to conceive who has not been taught about charting, give the gift of empowerment and share the FACTS about fertility with her! A good first step would be for her to learn how the signs of the female cycle relate to evidence based FABMs and then learn from an instructor trained in her method of choice!
Editor’s Note: Charting enables a woman to know and understand her body by tracking the physical signs of her cycle. This knowledge has applications for health monitoring as well as family planning. Physical signs that can be tracked include cervical fluid, basal body temperature, urinary metabolites, and cycle length. Learn more about charting on our website.
References
[i] Frank-Herrmann, P., et al. “Natural conception rates in subfertile couples following fertility awareness training.” Archives of Gynecology and Obstetrics, April 2017, www.ncbi.nlm.nih.gov/pubmed/28185073.
ABOUT THE AUTHOR
 Ana Maria Dumitru, PhD
Ana Maria Dumitru, PhD
Ana Maria Dumitru, PhD is an 8th year MD-PhD candidate at Dartmouth’s Geisel School of Medicine. She obtained her PhD in Biochemistry in 2017 and is in her final year of medical school at Dartmouth. She has served as a FACTS Student Ambassador for three years and is also trained as a FACTS Speaker.
Inspired by what you read?
You can support the ongoing work of FACTS here. To connect with a member of our team, please email development@FACTSaboutFertility.org. Interested in becoming an individual or organizational member? You can learn more and register here. To discuss with a member of our team, please email membership@FACTSaboutFertility.org.