By: Molly Marie Daley
This post is a brief synopsis of the article published in Osteopathic Family Physician by Manhart et al. It’s also the first post in a series we’re calling Featured Research, where we revisit a foundational research article in the field of fertility awareness. If you’re inspired to read the study in its entirety, please do! You can find it here.
Have you ever heard about fertility awareness-based methods of family planning (FABMs)? If you haven’t, you are not alone. Most people in the United States remain unfamiliar with or misinformed about FABMs.
FABMs teach women about their fertility and can be used effectively for family planning both to avoid and achieve pregnancy. This review article highlights the best quality research studies and the effectiveness rates for avoiding pregnancy for the different types of FABMs
Over three-fourths of reproductive-aged women in the United States ask their primary care clinicians about family planning services. It is often with a great amount of care (and hopefully an equally great amount of research) that women choose which method to use. And many women want to know about methods that have limited side-effects. In fact, one in five women in the United States expressed interest in using FABMs when given information about them[1].
How do FABMs work?
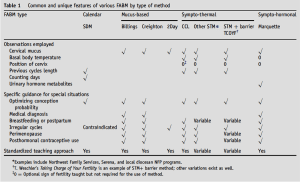
FABMs work with women’s natural cycles. Women who use FABMs learn to make observations about their body to determine whether they are fertile or infertile on any given day. (Women can only achieve pregnancy when they are fertile, which is usually during a 6-day window per menstrual cycle.[2]) When a woman is seeking to avoid pregnancy, she knows to avoid intercourse during her fertile period (and also that she can confidently engage in sexual intercourse during her infertile period). The different FABMs teach women to observe different signs (or a combination of them). There are four main categories of FABMs: (1) calendar-based; (2) mucus-based; (3) sympto-thermal; and (4) sympto-hormonal.[3] A woman who uses a FABM has the freedom to choose whichever method works best for her, given her preferences and lifestyle.
Are FABMs as effective as hormonal birth control?
Yes. High quality studies prove that FABMs can be as effective as hormonal birth control. SORT (Strength of Recommendation Taxonomy) is a process of assessing research quality and the strength of a body of evidence. It is basically a measure of how much weight a body of research has, how trustworthy the results are.

Due to the nature of FABMs, user participation and knowledge is required for effective use. This means that FABMs do not easily lend themselves to randomly controlled trials, partially contributing to the lack of research available on FABMs.[4] In addition, most of the studies are poor quality and feature a limited generalization of findings. Nevertheless, “at least 1 well-conducted, robust, clinical trial…is documented for each of the major FABMs.”[5] Furthermore, these high quality studies each report that FABMs are highly effective in avoiding pregnancy; these studies show that FABMs can be as effective as hormonal contraception.[6] This strong evidence stands in stark contrast with the incorrect, but commonly reported, statistic that FABMs reports unintended pregnancy rates of “~25 per 100 woman years.”[7] This statistic is incorrect because it includes extensive data from self-devised methods and outdated methods, and as a result, does not accurately reflect the actual effectiveness of modern FABMs.[8]
What are the benefits of FABMs?
FABMs are easy to learn, cost-effective, and often include motivational and structural support for clients.[9] Additionally, FABMs not only empower couples to avoid pregnancy, but also assist couples in achieving pregnancy, diagnosing and treating infertility and other gynecologic conditions, and embracing the emotional and relational aspects of their sexuality.[10] Furthermore, since education, literacy, and even poverty are not barriers to learn them, FABMs can benefit diverse populations.[11] Thus, in order to help women make more informed decisions about family planning, healthcare professionals need to become more familiar with the evidence based methods and be able share this information with their clients.
Appendix of web resources
If you are interested in learning more about FABMs, here is a list of helpful appendix web resources provided in the paper:
Cervical fluid methods
Sympto-thermal method (STM)
Sympto-thermal method + barrier
Sympto-hormonal method (SHM)
Additional methods
- LAM, Standard Days, and TwoDay Method
- Georgetown Institute for Reproductive Health
Resources:
[1] Page 2
[2] Page 3
[3] Page 3
[4] Page 4; In fact, only 29 peer-reviewed clinical studies about this topic have been published since 1980 (Page 5)
[5] Pages 5-6
[6] Page 6
[7] Page 7
[8] Page 7
[9] Page 6
[10] Page 7
[11] Page 7
ABOUT THE AUTHOR
Molly Marie Daley
Molly Marie Daley received her bachelors degree in Religious Studies and Arabic from The College of William and Mary, and holds a Juris Doctor from The University of Maryland School of Law. Molly works as an advocate for fertility awareness and she now lives in the San Francisco Bay Area with her husband Nick. She can be reached at mollymdaley@gmail.com, on Facebook (Molly Daley), or on Twitter (@mollymdaley).
Inspired by what you read?
You can support the ongoing work of FACTS here. To connect with a member of our team, please email development@FACTSaboutFertility.org. Interested in becoming an individual or organizational member? You can learn more and register here. To discuss with a member of our team, please email membership@FACTSaboutFertility.org.




